Maine: CoverME publishes official 2026 ACA Open Enrollment report

via CoverME, Maine's ACA exchange...the full report is 30 pages long; I've cross-posted the most important/relevant portions here:
CoverME.gov’s fifth Open Enrollment as a state-based marketplace was impacted by several changes in federal policy, including Public Law 119-21 (H.R. 1), the Centers for Medicare and Medicaid Services’ (CMS) Marketplace Integrity and Affordability Final Rule, and the expiration of the Enhanced Premium Tax Credits (EPTC) on December 31, 2025. The CoverME.gov team was committed to communicating these federal changes and their implications to our consumers in a clear, timely manner, while making operational updates to maintain compliance with all federal and state law. With increasing costs for health insurance, new administrative requirements and stricter eligibility criteria, Maine’s marketplace saw a decrease in overall enrollments for 2026, while still managing to enroll more than 8,500 new consumers. Alongside our sister agencies within the Maine Department of Health and Human Services, our team has remained steadfast in efforts to make progress towards the State of Maine’s goal to provide comprehensive health coverage to all Maine people.
Our priority is and remains Maine consumers – our family, friends, and neighbors, who do not have access to job-based health coverage and are not eligible for other forms of coverage. Navigating the health coverage landscape on your own can be confusing and stressful – knowing where to go, who to trust, and how to compare and choose coverage so that you know it will cover what you need, when you need it. And often also looming is the challenge of figuring out how to afford coverage, which was heightened in 2026 due to the federal expiration of EPTC. When faced with increases in premiums, which in many instances resulted in a doubling and tripling of monthly costs, tens of thousands of Mainers made the difficult decision to drop coverage.
...OHIM remains tremendously concerned about the Mainers who dropped coverage entirely, and the likely thousands of CoverME.gov consumers who have enrolled in plans with premiums or deductibles that they cannot afford for the entire plan year. These Mainers span all age groups and live in all areas of the state. Their household incomes also vary widely. The detrimental impacts on these individuals and families extend beyond their personal health. The impact will have ripple effects on our local economies through increases in health care bad debt and charity care, negative impacts on the health of our workforce, and reductions in available dollars to spend on goods and services in our communities....
- New enrollees – More than 8,500 Maine residents who didn’t previously have insurance through the marketplace enrolled in coverage for 2026. While this is a decrease from the 11,000 new enrollees in 2025, it is a testament to the marketing and outreach efforts CoverME.gov undertook to reach and enroll new consumers in the midst of rising insurance costs and tightening eligibility for coverage and financial help.
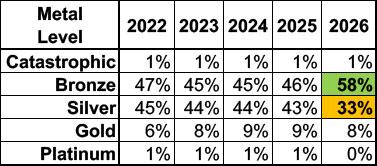
- More individuals enrolled in plans with higher out-of-pocket costs – Nearly 60 percent of enrollees selected Bronze plans for 2026, compared to just under 50 percent in 2025. Silver plans, which have higher monthly premiums but lower out-of-pocket costs for the consumer, saw enrollment fall by approximately 30 percent.
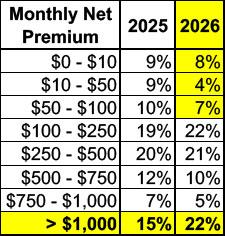
- Enhanced financial savings expired – Those who remain eligible for financial help are paying a similar net premium in 2026 compared to 2025. This is largely attributable to more consumers purchasing Bronze plans, and the overall CoverME.gov population having lower household incomes in comparison to the population enrolled last year. For those ineligible for financial assistance, monthly premiums rose by 33 percent. Furthermore, 22 percent of enrollees are paying more than $1,000 per month for their coverage (compared to 15 percent in 2025), and nearly 40 percent are paying premiums higher than $500 per month (compared to 33 percent in 2025).
...
- Over 58,000 Mainers, including more than 8,500 new consumers, selected health insurance plans through CoverME.gov during OE 2026.
- This is down approximately 24 percent from the more than 11,000 new consumers in 2025. Returning consumers who actively re-enrolled or were automatically re-enrolled in a plan represented the remainder, with a notable increase in active plan selections among re-enrollees. Specifically, over 50 percent of re-enrollees actively selected a plan, up from 33 percent in 2025, suggesting increased consumer engagement amid significant increases in premiums and more typical annual changes in plan options.
Enrollment of children (under age 21) declined at a faster rate than that of adults (aged 21+), likely as more children continue to be eligible for MaineCare.
With overall enrollment down in 2026, the numbers of both adult and child enrollees decreased. For children aged 20 and under, enrollments decreased nearly 14 percent. For adults aged 21 and up, enrollments decreased by just under 9 percent. Enrollees under age 21 have been steadily declining since 2023, when the state began implementation of the Maine Legislature’s expansion of eligibility for MaineCare (Medicaid) coverage for children under age 21. As described in more detail on page 12, the successful growth in young adult enrollment experienced in 2025 was short-lived. In recent years, CoverME.gov has focused targeted messages and marketing tactics on younger adult populations to help stabilize the risk pool and to lower uninsured rates among a population that has been historically challenging to enroll in coverage. Cost pressures of increased premiums during this OE likely contributed to younger adults having the greatest proportional declines of coverage, further skewing CoverME.gov membership to older age groups. As a result, the average age of consumers enrolled in health coverage through CoverME.gov increased from 42.9 years of age to 43.3 years of age.
Enhanced financial savings expired at the end Of 2025.
Some consumers were shielded from significant premium increases by original tax credits, while others saw significant increases in monthly premiums. For 2026 plans, the average premium for those receiving Advance Premium Tax Credits (APTC) through CoverME.gov remained consistent, despite overall gross premiums increasing by more than 20 percent. This is due to significant shifts into plans with lower premiums and higher cost sharing for health services, an increase in the proportions of lower-income enrollees, and shifts in the age distribution of consumers.
...During OE 2026, 58,523 Mainers selected health plans on CoverME.gov. Enrollment dropped by nearly 10 percent from OE 2025. This represents the lowest enrollment since Maine transitioned to a state-based marketplace.
The most populated counties - Cumberland and York - had the highest numbers of enrollments in the state. However, Knox County had the highest number of enrollments per capita, followed by Lincoln, Hancock, and Cumberland counties.
CoverME.gov members continue to be predominately female, and more than half of enrollees are over age 45. Enrollment by age demographics remained relatively consistent from 2025 to 2026. Two of the younger demographic groups - ages 0-17 and 25-34 - each saw a decrease of one percentage point from PY 2025. Two of the older demographic groups - ages 45-54 and 55-64 - each saw an increase of one percentage point. These changes are likely tied to the expiration of federal EPTC, increases in premium costs, and the historical trend of younger adults being more likely to go uninsured.
...A key feature of health insurance marketplaces is that premium and cost-sharing subsidies are available for some households, based on household income. These subsidies were more limited in OE 2026 due to the expiration of the EPTC, which were available from 2021 through 2025. This type of financial assistance helps individuals and families afford private health insurance coverage if they do not have access to affordable health coverage through an employer and they do not qualify for other health coverage programs, like MaineCare or Medicare. During OE 2026, nearly 3 out of 4 CoverME.gov enrollees who selected plans qualified for - and utilized – APTC to lower their monthly premiums. This was a decrease from 85 percent in 2025.
For enrollees receiving APTC, the average net monthly premium is $178. Without financial assistance, the average gross monthly premium for this group would have been $913. By comparison, the average monthly premium paid by members who do not receive APTC is $811. This represents an increase of more than 30 percent for those not receiving financial assistance in 2025.
...Except for Catastrophic coverage, health plans offered on CoverME.gov are categorized into four metal levels: Bronze, Silver, Gold, and Platinum. Higher metal level plans generally have a higher monthly premium but cover more of an individual’s out-of-pocket healthcare expenses. Metal levels indicate how consumers and insurance plans split the cost of health care expenses, with the higher metal level plans offering lower cost-sharing levels for consumers. This year, CoverME.gov saw plan selection shift significantly towards Bronze plans, which have higher out-of-pocket costs for consumers. CoverME.gov saw a 12-percentage point increase in Bronze plan enrollment and a 10-percentage point decrease in Silver plan enrollment.
...The expiration of EPTC in 2026 directly contributed to the increase in Bronze and Catastrophic plan selections, which may contribute to greater financial strain for Mainers. While some of those who purchase high-deductible plans can afford the deductible in the event they need significant health care services, it is likely that many of the households who moved into Bronze plans in 2026 made this choice because they could not afford higher premiums but wanted coverage to protect them from medical bankruptcy if faced with a serious health event or diagnosis.
If these families need health care services, they may not be able to pay the associated out-of-pocket costs, and may incur medical debt or seek hospital charity care. Increases in hospital bad debt and charity care will further strain Maine’s fragile health care system - especially in rural areas - and will result in higher health care costs for all Mainers.
...
During OE 2026, CoverME.gov recorded more than 8,500 plan cancellations. Around 5,000 of these cancellations were attributed to consumers relocating out of Maine or finding health coverage through another source such as an employer, Medicare, or MaineCare. However, nearly 3,500 discontinued coverage due to unaffordability of monthly premiums or another reason, suggesting they are going uninsured.
An analysis of cancellations cited for affordability reasons reveals a direct correlation with changes in financial help eligibility. Therefore, it is not surprising that most cancellations were among those who were eligible for financial help in 2025 but became ineligible in 2026. Specifically, those earning over 400% FPL – $62,600 annually for an individual and $128,600 for a family of four – represented nearly 40 percent of plan cancellations in 2026. These households became ineligible for any financial help available through CoverME.gov in 2026 due to the expiration of EPTC.
The affordability crisis for health coverage in 2026 is demonstrated throughout plan cancellation data. More than half of the consumers who cancelled health coverage for 2026 faced monthly premiums exceeding $750. Notably, the majority of these cancellations were seen with Bronze plans. As discussed earlier in the report, Bronze plans have relatively lower monthly premiums, with greater out-of-pocket costs and cost-sharing requirements. High rates of cancellations for Bronze plans are indicative of rising unaffordability across the health insurance marketplace, even for metal levels designed to offer lower monthly premiums.